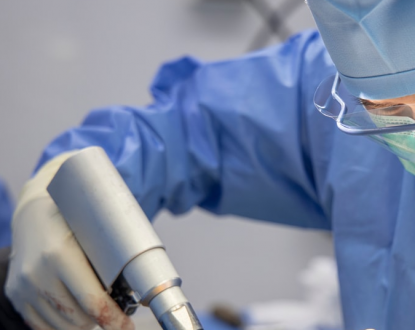
The Ludloff osteotomy is one of the surgical procedures that is performed to address a mild to severe hallux valgus abnormality. When examined in the sagittal plane, it appears as an oblique osteotomy of the first metatarsal. It was first explained by Dr. Ludloff in 1918.
In this procedure, the first metatarsal bone, which connects to the great toe, is sliced (osteotomized) in an oblique (slanted) fashion throughout the procedure. The bunion deformity is then corrected by rotating the bone after it has been sliced. In addition to this procedure, surgery to reposition the great toe itself is also performed. By first releasing and then tightening the great toe’s external joint capsule, this can be accomplished.
To accurately conduct the osteotomy, the surgeon must not only be able to complete the intricacies of the procedure, but they must also have an understanding of the constraints and risks of the Ludloff osteotomy.
For the Ludloff surgery to be successful, the cut bone must mend, which can take up to six weeks. During this period of recovery, it is typically not possible to place all of the weight on the foot. Instead, it is required to bear some weight through the heel and walk in a restricted manner while wearing a shoe or boot with a rigid sole.
The level of exercise can be increased once the bone has completely healed. It is essential to perform some specialized exercises regularly to keep the big toe joint mobile. It is common for patients to be able to return to their customary shoes between 8 and 12 weeks after surgery, and such shoes typically have a wider toe box.
Ludloff Osteotomy Indications
A hallux valgus deformity that has an intermetatarsal 1–2 angle that is greater than 15 degrees is the prerequisite for the Ludloff osteotomy. There are a few conditions that should not be treated with this procedure, including a narrow metatarsal that prevents adequate rotation of the dorsal fragment, first metatarsophalangeal arthritis that causes pain within the joint, and major first tarsometatarsal instability, and severe osteoporosis. Depending on the patient’s bone condition, the patient’s age of 60 years or more can be considered a relative contraindication. The quality of the bone in these patients is typically too low for this kind of osteotomy.
Ludloff Osteotomy Complications
Despite being rare, several problems are possible. These consist of:
- Infection
- Issues with wound healing
- Blood Clots: Pulmonary Embolism or Deep Vein Thrombosis (DVT) (PE).
Some other complications that might occur are as follows:
- In this procedure, injury to the medial branch of the superficial peroneal nerve, which transmits signals to the inside of the great toe, is possible. Furthermore, the deep peroneal nerve (which serves the region between the primary and second toes) is also damaged. These nerve injuries cause numbness or a burning-like discomfort. A complicated regional pain syndrome may very rarely arise as a result of nerve damage.
- The first metatarsal bone, which was sliced, could potentially mend very gradually or even not at all. It may need more surgery if it does not heal.
- When the bone recovers in an unsatisfactory position, this is known as a malunion. Additional surgery may be required in this case.
- After a Ludloff operation, the bunion deformity might occasionally recur. This might happen gradually over time or very quickly, and revision surgery is required in this case.
- An overcorrection of the bunion (also known as hallux varus), can occur post this surgery. This can result in excessive pain and deformity symptoms.
- Scarring may cause some loss of mobility in the big toe joint after surgery. Physical therapy can help with this. In some circumstances, the joint can eventually develop arthritis, necessitating additional surgery.
Ludloff Osteotomy Technique
Most of the time, the procedure is done while the peripheral nerves are numbed and the bleeding is stopped with a tourniquet. A tourniquet is not used in the majority of cases, which is believed to reduce postoperative edema.
Medially, a long incision is made from about midway up the proximal phalanx to about halfway down the first metatarsophalangeal joint. It is then cut horizontally immediately above the lateral sesamoid to remove the metatarsal-sesamoid ligament. The great toe is physically pushed into a 20-degree varus position after the lateral capsule is punctured at the first metatarsophalangeal joint line.
Typically, it is not essential to release the intermetatarsal ligament or the adductor tendon. One suture is put through the first metatarsal’s lateral aspect and the second’s medial periosteum. An osteotomy is complete when this suture is attached.
 Health & Care Information
Health & Care Information