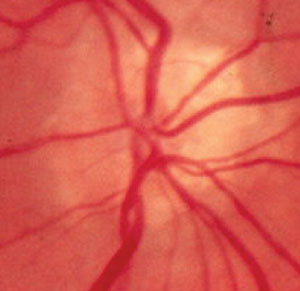
Pseudopapilledema is a medical condition that refers to the irregular elevation of one or both optic discs without edema of the retinal nerve fiber layer. The retinal fiber layer is formed; by optic nerve fibers expansion. The sparing of this layer is of vital importance in disease treatment; it serves as the basis for joining retinal prostheses to the optic nerve or implanting stem cells that may later regenerate the lost photoreceptors.
On the other hand, papilledema is different from pseudopapilledema. It is the swelling of the optic disc caused due to elevated intracranial pressure. It is essential to distinguish between the two. True papilledema is the first sign of a disease process with neurological impairment, the potential for vision loss, or death. Patients with papilledema are subjected to MRI, lumbar puncture, and extensive laboratory studies to find the cause. Therefore it is crucial to differentiate between the two and proceed accordingly.
Pseudopapilledema Symptoms
The symptoms of true papilledema differ from that of pseudopapilledema. Patients who tend to develop the condition of pseudopapilledema lack any visual symptoms. Patients affected with pseudopapilledema exhibit no obscuration of the vessels of the peripapillary region.
This condition may be bilateral or unilateral. However, the majority of its cases are bilateral. An extensive workup is unnecessary for the recognition of this condition. All it takes to diagnose pseudopapilledema is an experienced neuro-ophthalmologist or ophthalmologist who can correctly diagnose using ophthalmoscopic examination.
In patients affected with papilledema, the disc edema is secondary to increased intracranial pressure. It is also secondary to the optic disc drusen, also known as optic nerve head drusen or pseudopapilledema, an apparent optic disc swelling; it stimulates some features of papilledema but is secondary to a benign and underlying process. Papilledema patients exhibit vomiting, nausea, progressive headaches, positional headaches, transient visual obscurations, and binocular diplopia.
Pseudopapilledema Causes
Several causes can create pseudopapilledema. Small congenital nerves with a crowded optic nerve head can appear to have some mild elevation of the optic nerve head. These small-sized nerves are often visible in hyperopic eyes with shorter axial lengths. Conversely, in myopic eyes having longer axial length, the nerve may get inside the globe at an oblique angle; consequently, the nasal part of the nerve is more elevated than the temporal nerve.
Any irregularities around the optic nerve obscuring the nerve margins or elevating the nerve may produce this medical condition of pseudopapilledema. Those causes include; non-calcified, peripapillary astrocytic hamartomas or other peripapillary tumors and vitreopapillary traction.
Another variant, Burgmeister papillae, may originate from an imperfectly regressed hyaloid artery that may obscure the optic nerve, indicating papilledema. Abnormal migration of oligodendrocytes past the lamina cribrosa may also result in myelinated nerve fibers. It then causes the margin of the optic nerve to obscure.
Pseudopapilledema Diagnosis
It is significant that while diagnosing pseudopapilledema, it must remain distinguished from papilledema. A thorough physical examination distinguishes one condition from the other. However, sometimes this distinction is possible based on ophthalmoscopic findings.
In true papilledema, the peripapillary nerve fiber layer begins to swell. Fundoscopic examinations reveal the appearance of vessels in the peripapillary nerve fiber layer. It is the most distinguishing feature between the diagnosis of papilledema and pseudopapilledema.
Optical coherence tomography angiography is another diagnostic method that distinguishes pseudopapilledema from true papilledema. Patients with pseudopapilledema condition have eyes with a lower vessel density. Optical coherence tomography or OCT is another way that helps in diagnosing this medical condition. The peripapillary hyperreflective ovoid mass-like structure is sometimes visible in patients of pseudopapilledema. However, POHMS may also be visible in a wide variety of conditions; involving papilledema. Pseudopapilledema on the lumbar puncture reveals normal opening pressure opposite to the individuals with papilledema.
Pseudopapilledema Treatment
There are usually no recognized treatments for pseudopapilledema caused by the ODD or oppositional defiant disorder. Earlier, a case series investigated six patients with a severe field loss who underwent radial optic neurotomy. Those patients later found good results regarding the stabilization or improvement of visual function. The outcomes in this small series of patients were positive; the risks related to this surgery are such that it may be considered, in patients with visual loss, a typical finding in ODD. ODD complications must receive proper treatment as they occur. It is essential as no preventative measures are available for it.
There is usually no treatment necessary for pseudopapilledema if related to a congenital variant. However, if this condition is due to a peripapillary tumor, the treatment direction should be adequate. In patients with vitreopapillary traction, the traction may resolve spontaneously as the posterior vitreous detachment completes. If asymptomatic, pars plana vitrectomy may also be a therapeutic consideration.
 Health & Care Information
Health & Care Information