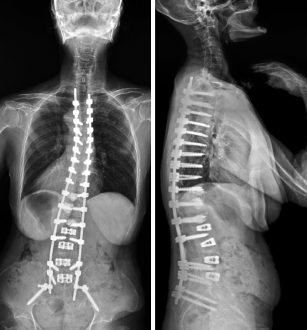
PJK is the most prevalent complication following a long instrumented posterior fusion in adult spinal deformity (ASD). Spine specialists defined the development of this abnormal kyphosis in various ways. The definition of PJK was first defined by Lee et al. and was commonly agreed upon by most specialists. According to him, a patient is said to have PJK when he/she with adolescent idiopathic scoliosis having kyphosis (5 degrees) higher than normal at the instrumented fusion’s proximal level usually appears shortly after the operation. According to the reported cases, several risk factors are responsible for the occurrences of PJK. Patients aged more than 55 years, the prevalence of compression fractures and loosening of the pedicle screw at the UIV due to osteoporotic bone, greater curvature correction, gender of the patient, and thoracic hyperkyphosis are some of the major risks associated with the kyphosis. Moreover, they may lead to revision surgery.
Now, the potential risk factors for PJK are recognized and acknowledged. Based on this analysis, a precise preoperative plan should be established to address and prevent proximal junctional kyphosis.
What is Proximal Junctional Kyphosis?
Proximal Junctional Kyphosis or forward curvature of the upper back (Kyphosis) is a common complication that develops in adult patients who undergo long posterior spinal surgery. This rate varies between 15% to 48%. However, several findings have shown that most cases occur within two years of spinal surgery, while two-third of the cases are reported within the first three months. PJK is known to be multifactorial in origin and is often diagnosed by radiography. The diagnosis of the PJK comprises a group of heterogeneous disorders, including acute pain, ambulatory difficulties, and in the most critical cases, neurological deficit. On the other hand, recent studies conclude Proximal Junctional Failure (PJF), the most progressive kyphosis, requires revised surgery for proximal extension of fusion.
Proximal Junctional Kyphosis – Symptoms
According to spine specialists, PJK is not an immediate symptom. It develops internally around the adjacent segment after the spinal fusion and is considered one of various ongoing adjacent segmental problems. It has also been studied that not all patients need revision surgery. Some PJK patients might not show any symptoms, whereas those with significant symptoms require surgical treatment. Even after various studies on PJK have been conducted, the experts hold a difference of opinion about the treatment and prevention of PJK. However, some studies have reported that the most influenced factors of proximal junctional kyphosis revision surgery are severe pain – especially if the patient is aged old, limb weakness, walking and balancing problems, neurologic deficit, and poor self-image.
Proximal Junctional Kyphosis – Causes
The causes of this devastating complication are not yet fully understood. However, it is believed that one or more of the following factors could be the reason for the development of this problem:
older age – may indicate poor quality of bones, the gender of the patient, fractures of the vertebrae, paraspinal musculature damage, large abnormal preoperative sagittal parameters, failure of lumbar spine instrumentation, degenerative disc disease (DDD), osteoporosis, low bone density, high body mass index, use of pedicle screws that increase the possibility of facet violation, disruption of posterior intervertebral elements, and impairment of the posterior soft tissues (posterior tension band, facet capsule, etc.) appear to be the increasing factors of PJK.
To reduce the occurrence of PJK in patients with pediatric deformities, a proper consideration of the above-mentioned causes/risk factors has to be done by the spinal surgeons.
Proximal Junctional Kyphosis – Treatment
As proximal junctional failure remains a challenging aspect of adult spinal deformity, several risk factors should be relatively considered before the surgery. PJK prevention strategies mainly focus on pre-operative planning, alignment, and steps to augment the upper-level fixation. These strategies can be applied, particularly in high-risk patients, to help reduce the rates of PJK.
The surgical techniques include the following:
- Take an entire spine lateral radiograph from a standing position
- Do a quick examination of bone mineral density before the surgery
- Check for sagittal alignment of a patient and conduct thorough revision by osteotomy
- Use of hooks in place of pedicle screws at the upper level since they provide a softer stress transition to the UIV
- The use of transition rods with a smaller diameter at the upper levels can minimize forces causing screw pullout or junctional stress
- Proper selection of the soft tissues around the UIV is very important
- Hook fixation and vertebral cement augmentation, when applied with novel strategies, have been shown to reduce the PJK rates.
 Health & Care Information
Health & Care Information