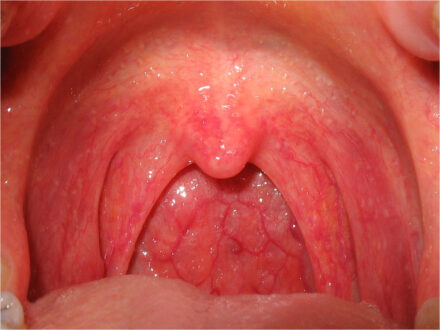
Learn all about pharyngeal erythema definition, symptoms, causes and treatment.
The 2000 National Ambulatory Medical Care Survey found that acute pharyngitis accounts for 1.1 percent of visits in the primary care setting and is ranked in the top 20 reported primary diagnoses resulting in office visits. Peak seasons for sore throat include late winter and early spring. Transmission of typical viral and GABHS pharyngitis occurs mostly by hand contact with nasal discharge, rather than by oral contact. Symptoms develop after a short incubation period of 24 to 72 hours.
Many things can cause inflammation to the throat area, including acid reflux and infections acid reflux of the stomach acid back up into the throat will injure the tissue surface/erode it with the strong acidic quality to the stomach fluids. This injury, especially over time, will cause inflammation and the redness/swelling of tissues. If acid reflux is constant, untreated/uncontrolled, long-standing/chronic, over years damage can occur to the esophagus lining.
The esophagus lining is normally lined with a certain type of cells (stratified squamous) much like your outer skin cells and are good for protection against environmental elements, however not great in sustained protection of high stomach acid elements. By the time you get to your stomach and remaining GI tract, the cell type changes and those cells (simple columnar mucus secreting) are able to survive and handle the constant acid changes/assault.
Viral throat infections do not require antimicrobial therapy and can be treated conservatively with supportive care. Acetaminophen or ibuprofen can be used for fever and pain management. Adequate oral hydration, frequent gargling, and over-the-counter anesthetic sprays and lozenges also may relieve the sore throat.
What is Pharyngeal Erythema?
Pharyngeal erythema is an acute infection of the pharyngeal mucosa caused by a variety of pathogenic microorganisms, the majority of which are viral. The lymphoid follicles of the throat are swollen and often covered with white exudate and cervical lymph nodes are enlarged and tender
Pharyngeal Erythema Definition
Pharyngeal relates to the pharynx part of your throat/oral cavity. Erythema is a description about redness of a tissue from inflammation (inflammatory chemicals increase blood flow to area, increase RBC’s and makes it appear red). Hence pharyngeal erythema is the inflammation of pharynx.
Pharyngeal Erythema Symptoms
Sore throat is the chief symptom in patients with viral pharyngitis. Patients may have additional symptoms that vary based on the causal pathogen. These symptoms are generally not useful in discriminating between the causes of viral pharyngitis because the symptoms produced by the numerous viruses that cause pharyngitis are so similar and commonly overlap each other. Sore throat is usually not the primary symptom. Nasal symptoms, such as sneezing, watery nasal discharge, nasal congestion, or postnasal discharge, tend to precede throat symptoms
Pharyngeal Erythema Causes
The majority of patients who present with a sore throat will have pharyngitis which is primarily caused by bacteria and viruses in the immunocompetent host. Bacterial etiologies of pharyngitis include Streptococcus pyogenes (or Group A streptococcus), as well as, Corynebacterium diphtheriae, Arcanobacterium haemolyticum, Neisseria gonorrhoeae, Group C and Group G streptococci and Mycoplasma pneumoniae. Viruses that cause pharyngitis include Epstein-Barr virus (EBV), herpes simplex virus (HSV), adenovirus, enterovirus, human immunodeficiency virus (HIV), cytomegalovirus (CMV), influenza and parainfluenza viruses. Pharyngitis due to viruses is often associated with respiratory symptoms such as rhinorrhea, nasal congestion and cough. Patients with pharyngitis due to GAS usually do not have cough or nasal symptoms.
Pharyngeal Erythema Treatment
Pharyngeal erythema treatment depends on the severity of condition. Antibiotic therapy decreases the duration of symptoms mildly, diminishes transmission, reduces the likelihood of supportive complications such as retropharyngeal and peritonsillar abscesses, and prevents the development of acute rheumatic fever if treatment is given within 9 days of onset of illness. First-line therapy for GAS pharyngitis continues to be penicillin, which may be given as a single intramuscular dose of benzathine penicillin G 600,000 units if <27 kg (60 lbs.) or 1.2 million units if >27 kg (60 lbs.). Oral penicillin VK 250 mg twice a day if <27 kg or 500 mg twice a day if >27 kg (60 lbs.) for 10 days also is considered first-line therapy.
Oral amoxicillin suspension is also commonly used as an alternative to oral penicillin because of its palatable taste and subsequent better compliance. Children with penicillin allergy can be treated with macrolides such as erythromycin, clarithromycin, and azithromycin (12 mg/kg per d for 5 d) as long as macrolide resistance has not been documented in the community. Cephalosporins and clindamycin are additional options if other first-line antibiotics are contraindicated. Clindamycin is effective also for the eradication of the carrier state in patients who continue to test positive for GAS despite treatment with penicillin. Patients with GAS pharyngitis are no longer considered contagious after 24 hours of antibiotic therapy.
 Health & Care Information
Health & Care Information