Learn all about Eczema Herpeticum and the symptoms of this condition. Whether it is contagious or not? Also about the treatments used to get rid of this disease. Eczema Herpeticum was first described by Moriz Kaposi in 1887. Fritz Juliusberg coined the term Pustulosis varioliformis acute in 1898. Eczema Herpeticum is a widespread, potentially serious viral infection of the skin. It can affect people most commonly with atopic eczema and other inflammatory skin conditions.
Eczema Herpeticum is a rare but severe disseminated infection that generally occurs at sites of skin damage produced by, for example, atopic dermatitis, burns, long term usage of topical steroids or eczema. It is also known as Kaposi varicelliform eruption, Pustulosis varioliformis acute and Kaposi-Juliusberg dermatitis. Most people with atopic dermatitis also have Staphylococcus aureus bacteria on their skin. The staph bacteria multiply rapidly when the skin barrier is broken and fluid is present on the skin.
Eczema Herpeticum is caused by Herpes simplex virus HV1, the virus that causes cold sores; it can also be caused by other related viruses. People with atopic eczema may experience perfectly ordinary cold sores, but rather than remaining confined to a small area of skin, the virus may infect large areas of skin. The reasons for this are not yet known. Eczema Herpeticum produces an itchy and sore skin eruption. It often causes high temperature and shivering, and makes you feel unwell. It may result in swollen lymph glands.
Atopic dermatitis (eczema) is a condition that makes your skin red and itchy. It’s common in children but can occur at any age. Atopic dermatitis is long lasting (chronic) and tends to flare periodically and then subside. It may be accompanied by asthma or hay fever. Atopic dermatitis most often begins before age 5 and may persist into adolescence and adulthood. For some people, it flares periodically and then clears up for a time, even for several years.
No cure has been found for atopic dermatitis. But treatments and self-care measures can relieve itching and prevent new outbreaks. For example, it helps to avoid harsh soaps and other irritants, apply medicated creams or ointments, and moisturize your skin. Patients with a history of recurrent HSV-1 or HSV-2 infection and a chronic skin disease which predisposes them to Eczema Herpeticum should be offered prophylactic antiviral therapy. Bacterial super infection should be addressed with oral antibiotics. Most commonly, Staphylococcus coverage is required (Brook, Frazier, & Yeager, 1998).
Is Eczema Herpeticum contagious?
Eczema is not contagious like the flu or a cold, but it is often inherited or passed through genes. The most common type of eczema, called atopic dermatitis, occurs in about 8 in 10 children where both parents have the condition and in about 6 in 10 children where one parent has the condition. However, if the raw, irritated skin of eczema becomes infected, the infecting agent may be contagious. The exact cause of atopic dermatitis is not known, but because it often occurs in family members, it is felt that a person’s inherited genes may play a role in its development.
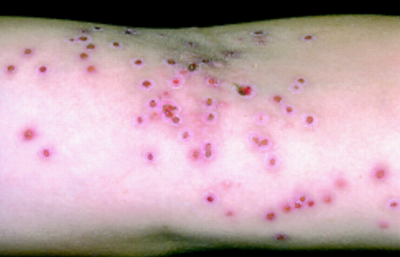
Eczema Herpeticum Symptoms
Eczema skin symptoms can be very mild. Some of the symptoms of Eczema Herpeticum are:
• Redness or skin discoloration
• Inflammation
• Scaling
• Thickening of the skin
• Oozing skin sores
• Crusting skin sores
• Itchiness
• Chronic and relapsing skin changes
• Xerosis (dry skin)
• Elevated Immunoglobulin E activity
• History of asthma or hay fever
• History of close relatives with eczema
• 5-12 days after exposure – Rashes with blisters at eczema lesions/skin patches
• Spreading of the blisters with yellow pus, accompanied with flu, fever and body aches
• Blisters start to get painful with bleeding, scabbing
• Widespread at body parts, usually neck, head, upper body with swollen lymph nodes.
Eczema Herpeticum Treatment
Eczema Herpeticum Treatment is considered as one of the few dermatological emergencies. Prompt treatment with antiviral medication should eliminate the need for hospital admission.
• Oral acyclovir 400 to 800 mg 5 times daily, or, if available, valaciclovir 1 g twice daily, for 10 to 14 days or until lesions heal. Intravenous acyclovir is prescribed if the patient is too sick to take tablets, or if the infection is deteriorating despite treatment.
The main treatments for atopic eczema are:
• emollients (moisturizers) used every day to stop the skin becoming dry
• topical corticosteroids creams and ointments used to reduce swelling and redness during flare-ups
Other treatments include:
• topical pimecrolimus or tacrolimus for eczema in sensitive sites not responding to simpler treatment
• antihistamines for severe itching
• bandages or special body suits to allow the body to heal underneath
• more powerful treatments offered by a dermatologist (skin specialist)
• Silver sulfadiazine is also recommended to prevent infection.
 Health & Care Information
Health & Care Information