Read about Cervical Radiculopathy Treatment: Surgery, Physical therapy. Cervical Radiculopathy exercise and symptoms.
Cervical radiculopathy, also known as pinched nerve occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal cord. It is the damage or disturbance of nerve function that results if one of the nerve roots near the cervical vertebrae is compressed.
Damage to nerve roots in the cervical area can cause pain and the loss of sensation along the nerve’s pathway into the arm and hand, depending on where the damaged roots are located. Cervical radiculopathy is a dysfunction of a nerve root of the cervical spine. The seventh (C7: 60%) and sixth (C6: 25%) cervical nerve roots are the most commonly affected.
Cervical Radiculopathy Treatment: Surgery, Physical therapy
Let’s review Cervical Radiculopathy Treatment: Surgery, Physical therapy.
Cervical Radiculopathy Causes
Spinal nerves can be impinged by:
- Arthritis or disc wear-and-tear with age
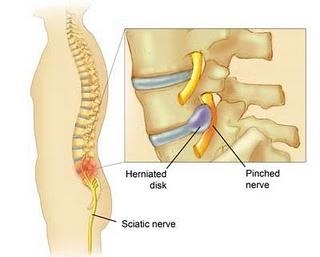
- Herniated or bulging discs from trauma or degeneration
- Spinal stenosis, which is a narrowing of the spaces in which the nerves travel
- Tumor, which can be benign or malignant, impinging the nerve root.
In middle-aged people, normal degenerative changes in the discs can cause pressure on nerve roots. In younger people, cervical radiculopathy tends to be the result of a ruptured disc, perhaps as a result of trauma. This disc material then compresses or inflames the nerve root, causing pain.
The main symptom of cervical radiculopathy is pain that spreads into the arm, neck, chest, upper back and/or shoulders. A person with radiculopathy may experience muscle weakness and/or numbness or tingling in fingers or hands. Other symptoms may include lack of coordination, especially in the hands.
Cervical Radiculopathy Treatment
Physical Therapy
Physical therapy is an effective treatment for cervical radiculopathy, and in many cases, it completely resolves symptoms. Physical therapist will develop an individual treatment plan based on the findings of patient’s initial evaluation. The treatment plan may include:
Pain Management
The first goal is to reduce the pain and inflammation in the area. Ice packs applied to the neck and scapular (shoulder blade) region during the first 24 to 48 hours following the onset of pain, help reduce inflammation. Moist heat can be used after this time period to help the surrounding muscles relax.
Physical therapist may advise to wear a soft cervical collar at times throughout the day, to allow the neck to relax. A cervical contoured pillow may be recommended to properly support the neck, and allow you to sleep more comfortably.
Manual Therapy
This includes manual cervical traction, to relieve pressure in the cervical (neck) region. This procedure can provide immediate relief of pain and numbness radiating into the arm.
Gentle massage may also be performed on the muscles of the cervical spine and scapular region. This technique helps the muscles relax and improves circulation to the area, promoting healing and pain relief.
Posture Education
It is an important part of rehabilitation. Your physical therapist may suggest adjustments to your workstation and work habits, to promote good posture to protect your neck.
In the early stages of recovery this may mean sitting only 15 to 20 minutes at a time. You will also receive instructions on how to bend, reach, and lift throughout the day in safe positions that place minimal pressure on your spinal discs.
Range of Motion Exercises
Gentle cervical mobility exercises are recommended to relieve symptoms and allow returning to normal movement. In the beginning stages of recovery, it is important that none of these exercises increase the pain radiating down into your arm.
It is important to communicate your symptoms accurately to physical therapist. If you spend many hours sitting at a desk during your workday, your neck may become stiff, physical therapist will teach neck stretches to take pressure off of your neck from extended periods of sitting and to help improve your mobility.
Strengthening Exercises
Physical therapist will help to determine which muscle groups need to be strengthened based on which spinal nerves are involved in particular case. When pain no longer radiates down to arm, more aggressive strengthening exercises are useful to be done.
Functional Training
As symptoms improve, physical therapist will work on functional exercises to help you return to your job, sport, or other daily activities. For example, if your job duties require overhead reaching, pushing, pulling, and long periods of sitting, you will be taught ways to perform these tasks to reduce undue stress to the neck.
Surgery
Most people with cervical radiculopathy get better without surgery. In rare cases, people don’t get relief with nonsurgical treatments. They may require surgery. There are several types of surgery for cervical radiculopathy. These include
- foraminotomy
- discectomy
- fusion
Foraminotomy
A foraminotomy is done to open the neural foramen and relieve pressure on the spinal nerve root. A foraminotomy may be done because of bone spurs or inflammation.
Discectomy
In a discectomy, the surgeon removes the disc where it is pressing against a nerve. Surgeons usually perform this surgery from the front (anterior) of the neck.
This procedure is called anterior cervical discectomy. In most patients, discectomy is done together with a procedure called cervical fusion.
Fusion
A fusion surgery joins two or more bones into one solid bone. The purpose for treating cervical radiculopathy with fusion is to increase the space between the vertebrae, taking pressure off the nerve. The surgery is most often done through the front of the neck.
After discectomy (taking out the disc), the disc space is filled in with a small block of bone graft. The bone is allowed to heal, fusing the two vertebrae into one solid bone. The space between the vertebrae is propped and held open by the bone graft, which enlarges the neural foramina, taking pressure off the nerve roots.
 Health & Care Information
Health & Care Information 

