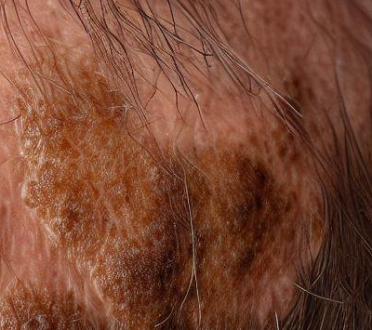
Erosive Pustular Dermatosis of the Scalp
EPDS is an uncommon inflammatory scalp disease that presents with thick crusts, skin atrophy, and erosions that leads to permanent hair loss.
Chronic scalp and leg skin inflammation is known as erosive pustular dermatosis (EPD). Bumps, sores, scabs, and pustules are its symptoms. It affects women more than males. The elderly are most frequently affected by EPD.
Elderly people with sun-damaged, bald scalps are more likely to develop erosive pustular dermatosis, which manifests as localized pustules, pus lakes, or crusts that cover eroded plaques or nodules. Erosive pustulosis is another name for erosive pustular dermatosis.
Males and females are both susceptible to developing erosive pustular dermatosis; the majority of patients are over the age of eighty. It generally manifests in scarred areas, such as those caused by traumas, or skin cancer treatments. Like other neutrophilic dermatoses, it is sometimes more prevalent with rheumatoid arthritis, myeloid hematological, and immune suppression diseases.
Erosive Pustular Dermatosis of the Scalp Symptoms
EPDS does not exhibit any well-defined symptoms. Pain and itching are occasionally reported by certain persons, but this is uncommon. Its frequency and prevalence are unknown because of its rarity. Clinically, pustules and erythematous skin erosion with thick crusts together with baldness, are the hallmarks of a condition known as erosive pustular dermatosis of the scalp.
In most cases, erosive pustular dermatosis begins as a cluster of very small pustules on the forehead, temples, or scalp. The lower legs are reportedly also affected. Lakes of pus, yellow-brown, or greenish crusts form as the pustules develop. After removal, the skin appears red and wet. Scarring and significant hair loss are two potential side effects associated with this severe disease.
Erosive Pustular Dermatosis of the Scalp Causes
Erosive Pustular Dermatosis is often caused by solar damage or skin injury, such as by medical or surgical procedures. It’s not infectious, contagious, or malignant. Most of the time, it happens on its own, but it has been linked to several other diseases, including arthritis, blood problems, inflammatory bowel disease, and thyroid disease.
This syndrome is commonly caused by pathergy, a minor skin injury (including surgery), and poor wound healing. Due to the lesions’ resistance to antibiotic treatment, infection is not assumed to be the underlying cause. Edema and venous stasis are possible contributors when it occurs in the lower legs.
Erosive Pustular Dermatosis of the Scalp Treatment
Therapy for this condition mostly starts with good local skincare, which includes daily dressings and the delicate removal of crusts. EPDS is uncommon and its cause is unknown, hence there is no standard advice for treatment. However, topical medicines are the most common and first-line treatment. Reduce inflammation, mend erosions, and stop scarring alopecia with early therapy to avoid irreversible hair loss. The treatment for EPDS needs to be prolonged and last for several weeks to months.
Treatment options include dapsone gel, photodynamic therapy (PDT), oral zinc sulfate, silicone gel, retinoids, topical retinoids, retinoids, and calcipotriol. First-line treatments that encourage re-epithelialization include tacrolimus, wound dressings, and corticosteroids.
The most popular form of treatment for this condition is high-potency topical corticosteroids, which are well-researched to be both efficient and safe. The potential for skin shrinkage and EPDS relapse upon treatment withdrawal are two drawbacks of topical steroids. The use of steroids needs to be stopped if no improvement is seen after the first two months.
Other effective treatments include:
- Anti-inflammatory medicines like minocycline for six weeks.
- Calcipotriol cream to lessen scaling.
- Cryotherapy for actinic keratoses.
- Zinc sulfate.
- Acitretin, isotretinoin, and oral retinoids.
Erosive pustular dermatosis can return after successful treatment. After checking any underlying skin malignancies, repeat the same treatment.
In conclusion, medical pharmacological therapy for EPD has mixed results, requiring long-term treatment, especially with topical treatments, and there is a higher chance of relapses. Therefore, topical calcineurin inhibitors are indicated for maintenance.
 Health & Care Information
Health & Care Information