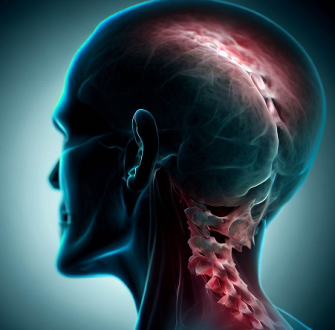
What is Cervicocranial Syndrome?
The skull and cervical spine form the craniocervical junction. Cervicocranial Syndrome, also known as Barre-Lieou Syndrome or Craniocervical Junction Syndrome, is a set of symptoms produced by an injury, sickness, degeneration, or a combination of these.
This syndrome can result from displaced, compressed, or misplaced cervical vertebrae (C1-C7). The most often damaged areas are typically the higher cervical vertebrae and occiput, which are mostly seen by imaging tests like an MRI. These anomalies lead cervical spinal nerves to malfunction, interrupting brain-brain stem-body communication.
Cervicocranial syndrome can develop as a consequence of neck ligament weakness. Most individuals spend a lot of time staring down at their phones and hunched over at their laptops, which weakens their neck ligaments. Their profession includes writing on their computers or being constantly linked to their mobile phones for many hours every day, as well as the massive increase in computer gaming.
Definition
Cervicocranial syndrome is a neurological illness that is caused by an abnormality in the neck, specifically the cervical vertebrae (C1 – C7). It is also known as Craniocervical Junction Syndrome or Barre-Lieou Syndrome.
Cervicocranial Syndrome Symptoms
A complicated collection of neurological symptoms is referred to as cervicocranial syndrome, which is also referred to as the Barre-Lieous syndrome. The course of the symptoms and signs of anomalies at the craniocervical junction can differ and can follow a minor neck injury or develop spontaneously. The presentation differs depending on the amount of compression as well as the structures that are affected.
Constant pain in the head, neck, face, sinuses, ears, and carotid arteries are typical symptoms. Some individuals also report a persistent, dull, throbbing pain at the base of the cranium that is exacerbated by head or neck movement. Neck discomfort and headaches frequently intensify with the movement of the head and are often triggered by coughing or leaning forward. The following are a few additional symptoms:
- Sinus congestion.
- Crepitus sound in the neck.
- Syncope.
- A loss of vision.
- An unconscious eye movement.
- Tinnitus.
Cervicocranial Syndrome Causes
Congenital or acquired factors can cause the craniocervical syndrome. Congenital craniocervical junction anomalies can be structural or general or systemic illnesses that influence skeletal growth and development. Multiple abnormalities are common in many patients.
The cervicocranial syndrome can be caused by a defect (a genetic mutation or the development of diseases later in life) or by an injury to the neck, more specifically the cervical region, which causes damage to the spinal neurons that are traveling via the cervical region and ultimately results in vertebral subluxation. Examples of situations that might lead to cervicocranial syndrome include vehicular accidents, trauma, osteoarthritis, tumors, degenerative disease, and other numerous causes of spinal instability.
Injuries and diseases are among the acquired causes of the craniocervical junction. For instance:
- Most disease causes are rheumatoid arthritis.
- Atlantoaxial dislocation, basilar invagination, and platybasia can result from cervical Paget disease.
- Metastatic bone tumors can cause atlantoaxial dislocation.
- Craniocervical junction tumors that grow more slowly (for example, meningiomas and chordomas) have the potential to press on either the brain stem or the spinal cord.
- Accidents, falls, and diving can cause bone, ligament, or both injuries, some of which are deadly.
Cervicocranial Syndrome Treatment
The primary function of treatment is symptomatic because cervicocranial syndrome predominantly affects the biomechanical components of the disorder. Medication does not affect cervical disc volume or uniformity. The syndrome-related deep and severe pain, however, is found to be efficiently relieved by medicine.
Prescription sedatives and tranquilizers are sometimes given to people who suffer from chronic nighttime pain and central sensitivity to biomechanical stress. It’s important to keep in mind that medicine should be used in addition to physical therapy and that educating the patient is the best way to stop misuse and the risks that come with it.
When cervicocranical syndrome is caused by a genetic mutation and runs in families as a result of other co-morbidities, genetic counseling can assist patients understand the dangers, prevention, and expectations of caring for and passing genes to a newborn.
The prognosis of a person with cervicocranial syndrome changes due to multiple factors, such as co-morbidities and traumatic events. A patient’s neurological integrity can be threatened by cervical spine instability. Cervical spinal surgery reduces symptoms.
 Health & Care Information
Health & Care Information