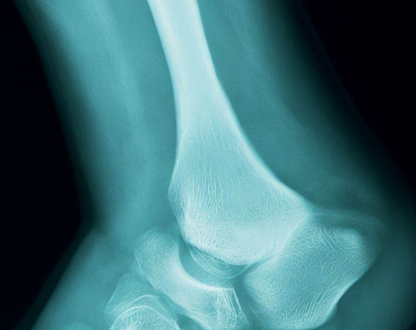
What is Mueller Weiss Syndrome?
A rare bone disorder characterized by the spontaneous onset of tarsal navicular osteonecrosis in adults. Patients mostly complain about midfoot and hindfoot pain that persists despite treatment, as well as midfoot edema and tenderness over the dorsomedial aspect, a collapsed medial longitudinal arch, and pes planovalgus. The comma-shaped deformity is shown on X-rays when the lateral aspect of the navicular bone collapses, causing the medial or dorsal aspect of the bone to protrude. This syndrome, which is associated with pathological fractures, can be bilateral or asymmetric. The most constant clinical symptoms of MWS (Mueller-Weiss syndrome) are a heel varus deformity and discomfort that occurs in the fifth decade.
Schmidt initially characterized the Mueller-Weiss disease in 1925. In 1927, W. Mueller was the first to postulate that this condition is triggered by either congenital abnormalities or compression on the tarsus. Based on radiographic results, radiologist K. Weiss first suggested in 1929 that this condition is caused by a lack of blood supply (an ischemic process). Thus, Mueller-Weiss syndrome was given its name in honor of the two researchers who discovered its pathogenesis. Misdiagnosis of this illness leads to ineffective treatment in many cases. Early identification and management of this condition can result in better outcomes by avoiding significant degenerative change.
Mueller Weiss Syndrome Symptoms
MWD is characterized by a mild discomfort that lasts for a long time, followed by severe pain that is not caused by trauma and that frequently makes it impossible to stand or walk. MWD often presents as persistent pain in the dorsal and peri navicular regions of the foot. Mueller-Weiss Syndrome (MWD) is frequently characterized by the lateral ankle joint’s instability and soreness around the peroneal tendons.
MWD can cause a wide range of physical symptoms, from severe pain in the middle of the foot that makes it hard to move to increase foot deformity that doesn’t hurt or cause any other symptoms. The paradoxical pes planus varus and the laterally pointed talar head are symptoms of the advanced stage of MWD.
Mueller Weiss Syndrome Causes
The actual cause is unknown to experts. However, they believe that it can be caused by the following reasons:
- A forceful compression or squeeze on the collection of bones in the midfoot (also known as the lesser tarsus).
- (Congenital) birth defect.
- Insufficient blood flow to the navicular bone (ischemia).
The navicular bone, located in the center of the foot, is a half-moon or boat-shaped bone. If it abruptly loses its blood supply, bone tissue begins to die, causing the joint to erode and the bone to eventually collapse.
Mueller Weiss Syndrome Treatment
Mueller-Weiss syndrome currently has no optimal treatment. The doctor mostly recommends nonsurgical therapy to enhance the quality of life if the disease and signs are in the early phases.
These can consist of:
- Ankle-foot orthosis.
- A short-term foot cast to prevent excessive foot movement.
- Customized insoles and footwear (orthotics) for pain alleviation and arch support.
- NSAIDs.
- Less physical exercise.
The doctors mostly recommend surgery if these treatments are ineffective in treating the pain or if the symptoms worsen over six months. If the condition has reached stage 2, it is frequently recommended.
The following procedures can be performed during the operation:
Talonavicular cuneiform arthrodesis: This operation is performed to relieve foot pain and restore arch support.
Grafting of bone: The doctor uses a portion of bone from the legs, ribs, or hips, to mend the broken foot bones in this treatment. In certain instances, donor bone can be utilized.
Joint fusion and other less frequent procedures exist to treat this disease. Physical therapy can help patients to get back on their feet after surgery, and it is necessary both before and after the procedure.
 Health & Care Information
Health & Care Information